 When it comes to interventional cardiology – that’s using balloon angioplasty* and metal stents to open up blocked coronary arteries – it seems that medical evidence is still taking a back seat to doctors’ deeply ingrained practice patterns. Case in point, a warning from the health journalism watchdogs at Health Beat:
When it comes to interventional cardiology – that’s using balloon angioplasty* and metal stents to open up blocked coronary arteries – it seems that medical evidence is still taking a back seat to doctors’ deeply ingrained practice patterns. Case in point, a warning from the health journalism watchdogs at Health Beat:
“Even though many well-designed clinical studies conclude that drug therapy alone can reduce the risk of heart attack and death in people with stable coronary artery disease just as well as more expensive invasive procedures, many cardiologists continue to use interventions like propping open blocked arteries with costly stents instead of first trying medication.”
Or, as the Los Angeles Times put it in a piece called Cardiologists Rush to Angioplasty Despite Evidence for Value of Drugs:
“You can lead a cardiologist to water but, apparently, you cannot make him drink.”
A recent study reveals that one-third of patients still do not receive optimal medical therapy, as reported in the Journal of the American Medical Association. And without sending the patient home from hospital with the necessary treatment plan to control risk factors such as high blood pressure, heart disease can be expected to progress. Cardiologist Dr. Barry Kaplan observes:
“The fact that clinical practice has not significantly changed in regard to the treatment of (balloon angioplasty) patients with better medical therapy is concerning.”
The researchers are not talking about patients like me who have suffered a heart attack because of a fully occluded coronary artery. We typically have necessary stents implanted, followed by prescribed medical therapy. Rather, studies involve those who have a partial blockage that impairs their ability to get around and carry out the normal activities of life. About 65% of balloon angioplasties are performed on such patients currently.
Some hospitals have in fact become angioplasty factories, as described by Consumer Reports Health in an article called Too Much Angioplasty. They’re called factories because the balloon angioplasty & stent procedure is used even when open heart surgery to bypass an occluded artery would be a better option. For example, angioplasty may be less effective in patients who have diabetes. People with diabetes appear to have greater benefit from bypass surgery, especially if there are two or three blood vessels involved.
Dr. Fred Edwards is medical director of the department of cardiothoracic surgery at the University of Florida in Jacksonville and director of the Society of Thoracic Surgeons Research Center. He warns:
“Sometimes patients have so many stents that later bypass surgery becomes impossible. That’s called a full metal jacket.”
Overuse of angioplasty has made national headlines this past year, with the Department of Justice and the Senate Finance Committee investigating incidences in which hospitals subjected hundreds of patients to needless angioplasty procedures.
But recent research suggests that the problem is not isolated to a few overzealous practitioners. Only half of procedures that used angioplasty to open narrowed arteries in non-emergency situations were clearly appropriate, according to a study of almost 500,000 cases published in July 2011 in the Journal of the American Medical Association.
The researchers also uncovered wide variation among hospitals; the rate of clearly inappropriate angioplasty procedures varied from less than 6% at some to greater than 16% at others.
One factor leading to the overuse of angioplasty is that the same doctors who perform the procedure often also act as gatekeepers for the patient’s cardiac care.
For example, patients often sign a consent form for balloon angioplasty even before going in for angiography, the definitive test for blocked arteries. Then, if the angiogram reveals blockages, the interventional cardiologist can recommend clearing them with balloon angioplasty and (often) a stainless steel coronary stent while the patient is still on the cath lab table.
The Consumer Reports Health article questions this practice:
“Convenient? Sure. But necessary? Usually not. In non-emergencies, you have time to consult with a heart surgeon and even your primary-care doctor to discuss the options and arrive at the treatment strategy that’s best for you.”
Most patients and doctors overestimate the benefits of angioplasty procedure, suggests a September 2010 survey of 153 patients and their physicians at a Massachusetts medical center. Just 63% of physicians knew that except in emergencies, angioplasties only ease symptoms. And even those who were up-to-date apparently often did not inform their patients: 88% of patients who consented to the procedure mistakenly believed it would reduce their risk of having a heart attack.
In a study of more than 23,000 U.S. Medicare claims, more than half of patients had angioplasty done without first undergoing standard testing to prove it was necessary. And the rate of those procedures has increased 300% over the last decade
A previous 2007 study called COURAGE enrolled 2,287 patients with stable coronary artery disease. Half were given balloon angioplasty plus optimal medical therapy and half were given only the medical therapy (including meds like statins to reduce cholesterol, beta-blockers, ACE inhibitors and diuretics to reduce blood pressure, and aspirin or other blood thinners to prevent excessive clotting).
Study author Dr. William Boden of the University of Buffalo School of Medicine and his colleagues reported that patients in the two groups had the same number of heart attacks and strokes after treatment.
The sole difference was that patients receiving only medical therapy had more frequent chest pains, called angina. Those pains were manageable, however. The COURAGE study was expected to make a big difference in how cardiologists treat patients with the disorder. Apparently it did not.
Even when the COURAGE results were first reported in 2007, some cardiologists were skeptical that the study would have much true impact on the practice.
Dr. Salim Yusuf, a Canadian cardiologist who has frequently argued that stents are overused, openly questioned whether things would actually change even given the compelling COURAGE evidence. As he told The New York Times:
“We’re going to have a hell of a time putting the genie back in the bottle. It’s a $15-$20 billion industry. You have huge vested interests that are going to push you back.”
But interestingly, it’s not just in cardiology where we find established treatment protocols that do not reflect evidence-based medicine.
For example, Dr. George Lundberg, MedPage Today’s Editor-at-Large, reminds us about studies from the 1940s and 1950s suggesting that rates of acute rheumatic fever following strep throat could be cut from 2% to 1% (not to 0%) by using antibiotics. So, antibiotics for strep throat became and remain the “standard of practice” to prevent rheumatic fever.
But the length of time a person with sore throat is symptomatic prior to recovery is four to seven days, whether or not strep is found and regardless of whether antibiotics are used. Dr. Lundberg warns:
“One million prescriptions for antibiotics for sore throat may prevent one case of rheumatic fever. But they may cause 2,400 cases of significant allergic reactions up to and including anaphylaxis, 50,000 to 100,000 cases of diarrhea, and some 100,000 cases of skin rash.”
Dr. Ed Pullen of Puyallup, Washington (practically in my neighbourhood) supports this caution with the example of a common medical condition: acute sinusitis. He writes in his blog:
“There is a lot of evidence suggesting that antibiotic treatment of acute sinusitis of less than 10 days duration usually resolves without antibiotic therapy in about the same number of days and with about the same severity of symptoms as with antibiotic therapy. The outcome of an episode of acute sinusitis that has not been present long is therefore about the same with or without antibiotic therapy.
“But antibiotic therapy itself can lead to significant morbidity, both the individual treated and to the larger community. Antibiotic complications like C. difficile related pseudomembranous colitis is becoming more common and antibiotic resistant. With essentially every antibiotic from amoxicillin to Levaquin, side effects are quite common.
“So physicians face the challenge of convincing patients who have been treated for their sinusitis with antibiotics for years and usually get well within days of treatment (as they would usually without treatment) that they are better treated with saline nasal rinse, analgesics and tincture-of-time.”
Meanwhile, the recent scandal around stent-happy cardiologists being investigated/fired for implanting unnecessary coronary stents (and, in some cases, charged and convicted for health care fraud) does not help allay suspicions in both professionals and patients alike that something is very wrong in the cath lab.
For example, clinical guidelines require that a coronary artery must be at least 70% blocked before a stent is appropriate to open it up (and most cardiologists consider anything less than 50% blockage to be “insignificant”) But court documents in the case of accused Maryland cardiologist Dr. Mark Midei allege that some of his patients were told they had coronary blockages in the 90% range, while a subsequent review of their records shows actual blockages closer to 10% or less.
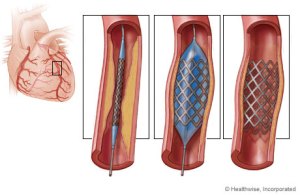
* Definition of angioplasty = the technique of mechanically widening a narrowed or obstructed blood vessel. An empty and collapsed balloon on a guide wire, known as a balloon catheter, is passed into the narrowed location and then inflated to a fixed size, crushing the fatty deposits that caused the blockage, and opening up the blood vessel for improved flow. The balloon is then deflated and withdrawn. Often, a stainless steel mesh coronary stent is implanted at the same time to help keep the newly-opened blood vessel stable before the catheter is removed.
NEWS UPDATE: July 14, 2011 – Baltimore, MD – “Cardiologist’s License Ordered Revoked In Stents Case” – A state medical panel has declined to reverse a judge’s order to revoke cardiologist Mark Midei‘s license on accusations he performed hundreds of medically unnecessary stent procedures. The Maryland Board of Physicians ruled that Midei violated five provisions of the Medical Practice Act, including provisions that prohibit unprofessional conduct, making false reports, keeping inadequate records and over-utilization of health care services. The board declined to reverse the ruling. The board considered Midei’s violations “repeated and serious”, further writing that Midei “unnecessarily exposed his patients to the risk of harm and increased the costs of the patients’ medical care.”
The judge had ordered Midei’s medical license be revoked and not reinstated for at least two years, to which the board agreed, adding that Midei had falsified the extent of blockages of patients’ coronary arteries by reporting them as being 80% blocked, when they were actually lower – and in most cases, much lower. In some patients, he had also falsely reported that they suffered from unstable angina when in fact they did not.
MORE STENT INVESTIGATIONS:
- March 3, 2011 – Medical reviews at Pittsburgh’s Westmoreland Hospital have determined two cardiologists there implanted coronary stents in at least 141 patients in 2010 who may not have had enough blockage in their arteries to need a stent. Letters to these patients do not provide a reason why the patients received the stents, but state their condition “may not have justified the placement of a coronary stent.” Hospital officials said the questionable stents were implanted by Drs. Ehab Morcos and George Bousamra, who voluntarily resigned their hospital privileges at Westmoreland on January 12, 2011 after being investigated. The two doctors performed more than 750 of the up to 2,000 stent procedures done at Westmoreland Hospital that year.
- July 26, 2011 – A federal jury has convicted Maryland interventional cardiologist Dr. John R. McLean, 59, on six charges of health care fraud relating to insurance claims he’d filed for stents deemed to have been placed unnecessarily, as well as for ordering unnecessary tests and making false entries in patient medical records. A statement released by the Office of the Inspector General said: “The evidence shows that Dr. McLean egregiously violated the trust of his patients and made false entries in their medical records to justify implanting unneeded cardiac stents and billing for the surgery and follow-up care.” McLean faces a maximum sentence of 10 years in prison for health care fraud and five years in prison on each of five counts of making false statements. His sentencing is scheduled for November 10, 2011.
- December 17, 2012 – Cardiologist Dr. Mehmood Patel began a 10-year prison sentence after the U.S. Court of Appeals, 5th Circuit upheld his 2009 conviction and rejected his request to reconsider.As reported by HeartWire, Patel, formerly of Our Lady of Lourdes Hospital and Lafayette General Hospital in Louisiana, was convicted on 51 counts of billing private and government health insurers for unnecessary coronary interventions and tests. During the criminal trial in 2008, the prosecution presented evidence that Patel falsified patient symptoms in medical records and billed more than $3 million over four years and kept over $500,000.
His lawyers tried to argue that criminal laws ought not to be applied to a doctor’s judgment.
.
See also:
- Did You Really Need That Coronary Stent?
- Stent-happy Docs on Notice in Maryland Health Care Fraud Debate
- Cardiologists Accused of Implanting Cardiac Stents That Weren’t Needed
- Doctors On The Take: How to Read the Fine Print in Medical Research Reports
Read more on the JAMA study from Naomi Freundlich‘s article in Health Beat.
.

Carolyn —
This is, of course, very disturbing information. One has to wonder why “scientists” — as doctors are trained to be — ignore evidence-based medicine.
After three stents — one which didn’t work and had to be redone, one which was botched and an artery was nicked, and one which may have caused a heart attack — I have to wonder about interventional medicine.
I would note that the emphasis on the articles is on taking drugs as being a better idea than stents — what ever happened to lifestyle changes as the most important thing one can do? Isn’t this part of the Big Pharma scam also?
Good point, Steve. If I were a skeptic (who, me?) I’d wonder if the Big Pharma manufacturers of statins, beta-blockers, ACE inhibitors and diuretics were somehow connected to this JAMA report. I’d also wonder if, once cardiologists have embraced new technology/devices/procedures, they may feel reluctant to suddenly stop doing them (like admitting that all those things may not have been necessary after all?) And patients tend to truly believe that more is better when it comes to medical procedures – particularly when it comes to vital organs like our hearts.
Yes there is a problem. Doctors are rewarded for expensive procedures, many patients like technology and lawyers rarely sue for “not doing something”. Articles like this hopefully educate the public that some medical technology is a bit like the emperors new clothes.
Lifestyle measures need to be number one in what is largely a lifestyle condition. Medications are number two, and intervention is for the minority who actually need it and will benefit.
“…Lifestyle measures need to be number one…”
But doesn’t this trend towards marketing-based medicine favour the passive patient whose preference is to meekly accept the prescription or procedure offered, not necessarily the one who will embrace exercise, healthy diet, stress reduction and other lifestyle improvements?
Procedural specialists earn more than medical practitioners who don’t perform procedures. It’s as fundamental as that.
I was a Registered Nurse, with considerable experience in a cardiothoracic unit. There is often a competitive, ego-driven culture between cardiologists and cardiac surgeons.
These days, I’m a natural medicine practitioner. I’m still waiting for the day when the risks associated with any number of so-called scientifically evaluated and validated medical drugs – some of them potentially life-threatening- are called something other than the innocuous blanket term of ‘side-effect’.
If I – and my peers – prescribed herbal preparations or gave acupuncture treatments which caused the following significant health concerns, or for which we charged our patients many thousands of dollars – there’d be a public outcry:
– deafness or tinitus- a common IV antibiotic, and any number of other drugs
– bone marrow suppression – many drugs
– myocardial failure – a class of chemotherapeutic agents {oncological drugs}
– kidney disorders or haemorrhage – certain over-the-counter NSAIDS { non-steroidal anti-inflammatories }
– psychosis – certain antimalarials
– peripheral neuropathy { nerve damage} – certain chemotherapeutic agents { oncological drugs}
I think it’s time we each asked of our medical practitioners: “Can you still promise me that your abiding commitment to me is that you will -as Hippocrates advised- first do no harm?”
Hi Margi,
Every drug – and every supplement – carries side effects. The question in evidence-based health care has always been: does potential good outweigh potential harm? This is true whether it’s a herbal supplement, an expensive drug or an invasive procedure like implanting cardiac stents.