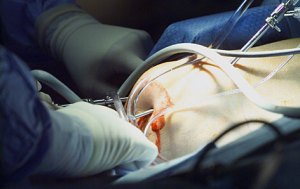
 When I had arthroscopic surgery on my right knee to repair a torn cartilage, my orthopedic surgeon also found evidence of osteoarthritis in that knee. Not surprising, really, given my age and family history, but new research says many docs would now be recommending drugs or surgery that they shouldn’t for that new diagnosis.
When I had arthroscopic surgery on my right knee to repair a torn cartilage, my orthopedic surgeon also found evidence of osteoarthritis in that knee. Not surprising, really, given my age and family history, but new research says many docs would now be recommending drugs or surgery that they shouldn’t for that new diagnosis.
This month’s issue of the journal Arthritis Care & Research suggests that doctors are disregarding standard medical guidelines to manage the joint inflammation condition of osteoarthritis (OA) through lifestyle improvements (like exercise or weight loss) – and instead relying on drugs and surgery.
Current management of OA typically relies on the use of anti-inflammatory and analgesic drugs. When symptoms become debilitating, even joint replacement is recommended, according to Dr. David J. Hunter of the University of Sydney in Australia.
Here in Canada, people with osteoarthritis are the most frequent users of non-steroidal anti-inflammatory drugs or NSAIDs – for example aspirin, Indocin, ibuprofen (Motrin), naproxen (Naprosyn), piroxicam (Feldene), and nabumetone (Relafen) – all of which can cause gastrointestinal (GI) bleeding – in itself a serious and sometimes fatal medical condition.
Age, heredity, obesity, or previous joint injury are considered common risk factors for OA. The 2008 Canadian Community Health Survey reported that about 16% of Canadians have this form of arthritis, with more women than men affected. That’s significantly less than the American rate, however, according to a previous study published in last February’s issue of Arthritis Care and Research. That study’s lead author Dr. Elizabeth Badley explained:
“Our study results suggest that the higher prevalence of arthritis in the U.S. may be a consequence of greater obesity and physical inactivity in that country, particularly in women.”
While lifestyle changes are apparently being overlooked in managing OA patients, medical imaging and surgery are relied on excessively, according to Dr. Hunter’s new research. The diagnosis of OA should be made clinically, not radiographically, he claims. In particular, magnetic resonance imaging (MRI) should be used only in the unusual situation where other more serious causes for joint pain need to be ruled out.
Dr. Hunter’s research shows that up to 50% of these high-tech MRI scans for OA done each year may be unnecessary.
Procedures such as joint replacement and knee arthroscopic surgery also should be avoided as much as possible. Joint replacement is effective but has risks, and arthroscopic debridement of the knee – the most common procedure done by orthopedic surgeons today – has “no demonstrable efficacy” for knee OA, the researchers stated. In analyzing potential strategies for improving quality, researchers suggested that changes be made to the medical education system to strengthen doctors’ adherence to standard, evidence-based guidelines.
Mayo Clinic experts recommend a lengthy list of preferred (and non-drug, non-invasive) suggestions to manage osteoarthritis, including:
- Rest: Rest sore joints for 12 to 24 hours. Find activities that don’t require you to use your joint repetitively. Try taking a 10-minute break every hour.
- Exercise: Get doctor-approved regular exercise when you feel up to it. Stick to gentle exercises, such as walking, biking or swimming. Exercise can increase your endurance and strengthen the muscles around your joint, making your joint more stable. But if you feel new joint pain, stop. New pain that lasts more than two hours after you exercise probably means you’ve overdone it.
- Lose weight: Being overweight or obese increases the stress on your weight-bearing joints, such as knees and hips. Even a small amount of weight loss can relieve pressure and reduce pain. Aim to lose 1 or 2 pounds a week, at most. Most people combine changes in their diet with increased exercise.
- Use heat and cold to manage pain: Both heat and cold can relieve pain in your joint. Heat also relieves stiffness and cold can relieve muscle spasms. Soothe your painful joint with warm – not hot – heat using a heating pad, hot water bottle or warm bath. Apply heat for 20 minutes several times a day. Cool the pain in your joint with cold treatments, such as with ice packs. You can use cold treatments several times a day unless you have poor circulation or numbness.
- Apply over-the-counter pain creams: Creams and gels available at the drugstore may provide temporary pain relief. Some creams numb the pain by creating a hot or cool sensation. Other creams contain medications, such as aspirin-like compounds, that are absorbed into your skin. Read the label so that you know what you’re using. Pain creams work best on joints that are close the surface of your skin, such as your knees and fingers.
- Use assistive devices: Assistive devices can make it easier to go about your day without stressing your painful joint. A cane may take weight off your knee or hip as you walk. Gripping and grabbing tools may make it easier to work in the kitchen if you have osteoarthritis in your fingers. Your doctor, occupational therapist, or medical supply catalogues have ideas about what sorts of assistive devices will be most helpful.
Read more about Dr. Hunter’s research in Docs Don’t Follow Osteoarthritis Guidelines.
.

“…arthroscopic debridement of the knee – the most common procedure done by orthopedic surgeons today – has “no demonstrable efficacy” for knee OA..”
Perfect timing. My doctor is aggressively recommending knee surgery for recently diagnosed osteo. I have a strong family history (mother, sisters, aunts). But my cousin three states away, however, with the same diagnosis is on a totally different track. Her doctors right away ORDERED (end of conversation – they mean business!!) weight loss and daily physical exercise like AquaFit pool exercises and physiotherapy. No mention of “arthroscopic debridement” of her knees. I’m going to bring this article to my own doctor, and send it to every other woman in my family who by now believe that knee surgery is just “how it’s done” for osteo. No more!!
Thank you Carolyn for this information.
I agree with MDuffy – even though I have virtually no symptoms, my doctor referred me to an orthopaedic surgeon to discuss arthroscopic knee surgery for my OA. Neither mentioned loosing weight (I’m down 12 pounds already with 18 more to go and so I told both of them that we can talk more AFTER I’m down to my ideal weight for my height).
Neither were happy AT ALL about my decision to simply try weight loss and increased exercise instead of heading to the O.R. There’s just more money to be made doing surgery than if the patient becomes responsible for her health with lifestyle improvements, I guess.
Juanita I think you are on the right track. My orthopod refused to book my knee surgery UNTIL after I lost 20 lbs first. He says having knee surgery but carrying around the equivalent of a huge bag of potatoes pounding on that injured knee every step is not a good predictor of surgical success. The odd thing: after I lost 22.5 lbs, my knee pain virtually disappeared on its own and no surgery was necessary after all! 🙂